Medicaid Enrollment Increases, Partly Due to the Federal Affordable Care Act (ACA)
- In January 2014, the State’s health insurance exchange, authorized by the ACA, took over from local districts the processing of most new Medicaid applications. The exchange averaged over 1.2 million Medicaid enrollees per month in SFY 2014-15.
- Compared to last year, average monthly enrollment* for:
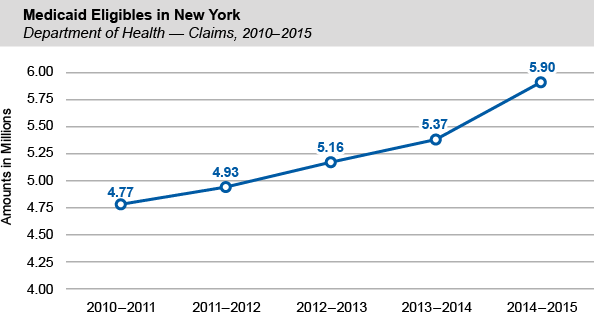
- overall recipients increased by 530,375 (9.9 percent) to 5.9 million, a portion of which is due to the enactment of the ACA;
- adults increased by 280,178 (13.6 percent) to 2.3 million, accounting for the largest increase in enrollment;
- children with Medicaid coverage increased by 225,754 (11.3 percent) to 2.2 million;
- elderly recipients increased by 10,893 (2.3 percent) to 485,655;
- blind or disabled recipients decreased by 6,094 (0.8 percent) to 773,627; and
- “other” eligible recipients, largely legal immigrants, increased by 19,644 (37.7 percent) to 71,771.
- Medicaid recipients in managed care plans increased by 433,126 (10.7 percent) to nearly 4.5 million. This increase reflects the enrollment of most new recipients into managed care plans and the continued transition of most populations from fee-for-service to Medicaid managed care.
Medicaid Spending Increases, Largely Due to Additional Federal Payments From the ACA
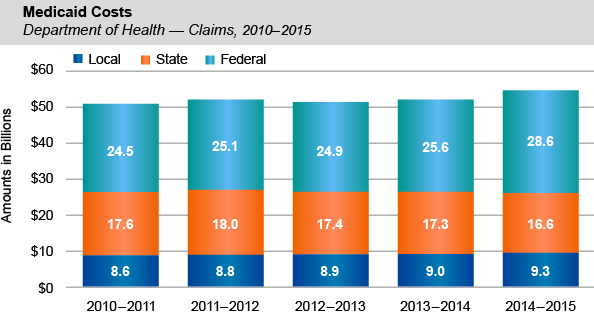
- Compared to last year, combined local, State and federal spending on Medicaid claims increased by $2.6 billion (5.1 percent) to $54.5 billion. This increase largely reflects additional federal Medicaid payments associated with the ACA.
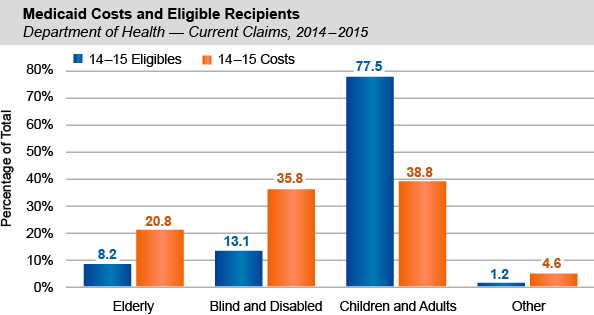
- Children and adults represented over three-quarters of all average monthly enrollees, but only 38.8 percent of the overall costs of Medicaid claims for the State.** Elderly, blind and disabled enrollees made up less than a quarter of eligible recipients, but accounted for 56.6 percent of Medicaid claims costs.
Family Health Plus Program Ends
- Under ACA reforms, the Medicaid expansion program Family Health Plus ended in December 2014. Family Health Plus provided coverage for certain adults who did not have health insurance and earned too much to qualify for regular Medicaid.
- The State transitioned most Medicaid enrollees to managed care and instructed those with income above the eligibility level to apply for non-Medicaid coverage through the State’s health insurance exchange.
- Compared to last year, in Family Health Plus:
- average monthly enrollment decreased by about 270,000 (66.1 percent) to 138,786; and
- year-to-year expenditures decreased by $1.1 billion (67.5 percent) to $545.1 million.
*Unreconciled paid claims from the Department of Health. SFY 2014-15 enrollment numbers are through February 2015.
**SFY 2014-15 costs by eligibility category (i.e., children, adults, elderly, blind and disabled) are through December 2014.